Emerging Concepts for Supporting Better Sleep in People With Sleep Apnea
Sleep apnea research is expanding, with specialists exploring how airway support, breathing patterns, and lifestyle adjustments may affect sleep quality. Advances in monitoring devices, sleep-position strategies, and environmental modifications are being evaluated to help individuals better understand their nighttime patterns. This article reviews the current ideas gaining traction as part of ongoing studies into sleep-related breathing issues.This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
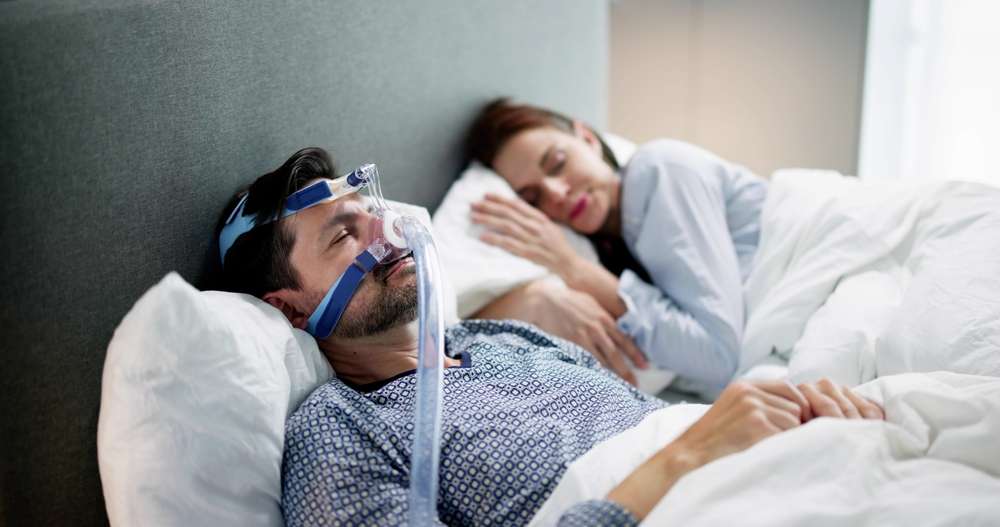
Sleep apnea represents one of the most prevalent sleep disorders in the United States, characterized by repeated interruptions in breathing during sleep. These episodes can occur dozens or even hundreds of times per night, leading to fragmented sleep, daytime fatigue, and various health complications. As our understanding of sleep apnea deepens, healthcare professionals are developing more comprehensive approaches that extend beyond traditional treatment methods.
Advancing Sleep Apnea Insights Through Modern Research
Recent research has revealed that sleep apnea involves complex interactions between anatomical factors, neurological control mechanisms, and environmental influences. Scientists are now investigating how genetic predisposition, muscle tone variations, and airway structure contribute to breathing interruptions. These insights are helping clinicians develop more personalized treatment strategies that address individual patient characteristics rather than applying one-size-fits-all solutions.
Studies have also shown that sleep apnea severity can fluctuate based on factors such as sleep position, seasonal changes, and even stress levels. This variability has prompted researchers to explore adaptive treatment approaches that can respond to changing conditions throughout the night.
Innovations in Breathing Support Research
The field of breathing support technology continues to evolve with promising developments in device design and functionality. Researchers are working on next-generation positive airway pressure devices that offer improved comfort, reduced noise levels, and enhanced user compliance. Some experimental devices incorporate artificial intelligence to automatically adjust pressure settings based on real-time breathing patterns.
Additionally, alternative approaches such as oral appliance therapy are being refined through advanced materials and custom-fitting techniques. These devices work by repositioning the jaw and tongue to maintain open airways during sleep, offering a less intrusive option for certain patients.
Neurostimulation therapy represents another frontier in breathing support research. This approach involves implanting small devices that stimulate specific nerves controlling airway muscles, helping maintain proper breathing patterns during sleep.
Optimizing Sleep Environment Adjustments
The sleep environment plays a crucial role in managing sleep apnea symptoms. Research indicates that factors such as bedroom temperature, humidity levels, and air quality can significantly impact breathing patterns during sleep. Optimal room temperature typically ranges between 60-67 degrees Fahrenheit, while humidity levels should be maintained around 30-50 percent to prevent airway irritation.
Bed positioning and elevation strategies are also gaining attention as supportive measures. Elevating the head of the bed by 4-6 inches can help reduce the severity of breathing interruptions by utilizing gravity to keep airways more open. Specialized pillows and positioning devices are being developed to maintain proper alignment throughout the night.
Air filtration systems and humidifiers can help create cleaner, more comfortable breathing conditions. Some patients benefit from removing allergens and irritants from the bedroom environment, which may reduce inflammation in the airways.
Enhancing Nighttime Monitoring Technologies
Advanced monitoring technologies are revolutionizing how healthcare providers track and assess sleep apnea. Wearable devices now offer continuous monitoring capabilities that can detect breathing patterns, heart rate variations, and sleep stages without requiring overnight laboratory stays. These devices provide valuable data that helps clinicians adjust treatment plans more precisely.
Smart home integration allows for comprehensive sleep environment monitoring, tracking factors such as room temperature, noise levels, and air quality alongside physiological measurements. This holistic approach helps identify environmental triggers that may worsen sleep apnea symptoms.
Mobile applications connected to monitoring devices enable patients to track their progress and share data with healthcare providers remotely. This connectivity facilitates more frequent treatment adjustments and improved patient engagement in their care.
| Technology Type | Provider Examples | Key Features | Cost Estimation |
|---|---|---|---|
| Advanced CPAP Devices | ResMed, Philips Respironics | Auto-adjusting pressure, data connectivity | $800-$3,000 |
| Oral Appliances | SomnoMed, ProSomnus | Custom-fitted, adjustable positioning | $1,500-$4,000 |
| Wearable Sleep Monitors | Oura Ring, Fitbit, WHOOP | Continuous tracking, smartphone integration | $200-$500 |
| Smart Air Quality Systems | Dyson, Honeywell, Molekule | HEPA filtration, humidity control | $300-$800 |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Implementation and Patient Considerations
Successful implementation of these emerging concepts requires close collaboration between patients and healthcare providers. Treatment plans should be individualized based on sleep study results, anatomical factors, lifestyle considerations, and patient preferences. Regular follow-up appointments allow for treatment optimization and adjustment of supportive measures.
Patient education plays a vital role in treatment success. Understanding how different factors affect sleep apnea helps individuals make informed decisions about lifestyle modifications and treatment adherence. Support groups and educational resources can provide additional guidance and motivation.
Healthcare providers emphasize that while these emerging concepts show promise, they should complement rather than replace established treatments. The most effective approach often involves combining multiple strategies tailored to individual patient needs.
The landscape of sleep apnea management continues to evolve as researchers develop new technologies and refine existing approaches. These emerging concepts offer hope for improved sleep quality and overall health outcomes for the millions of Americans living with sleep apnea. By staying informed about these developments and working closely with healthcare providers, patients can explore options that best suit their individual circumstances and preferences.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.




